Heparin versus Warfarin for Lupus
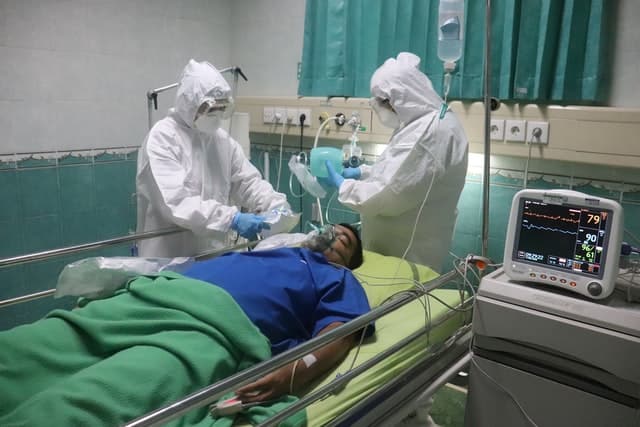
Systemic lupus erythematosus (SLE) can lead to blood clots through various mechanisms. In addition, lupus patients are at higher risk of heart attacks and strokes. Therefore, drugs that thin out the blood (anticoagulants) are often needed. Heparin and warfarin are …