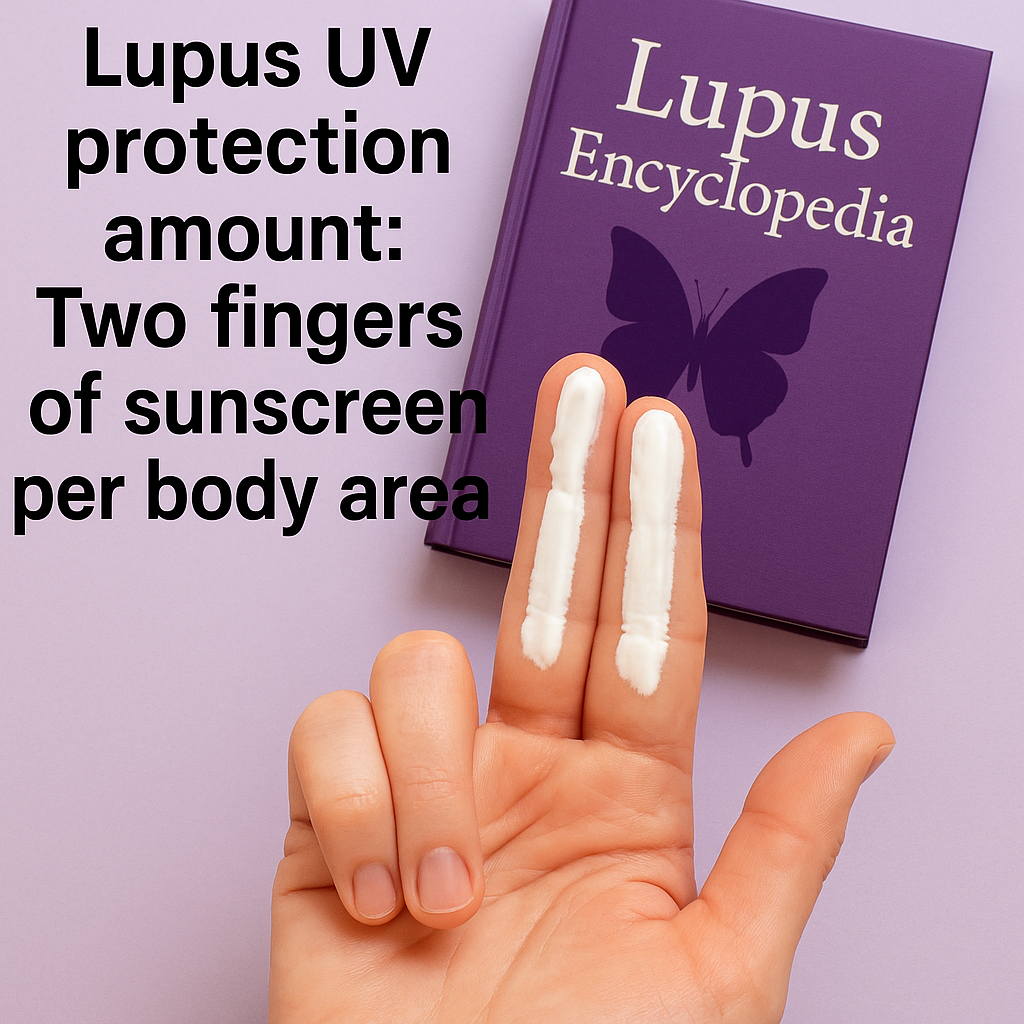
Sun Protection for Lupus Made Simple
SSun protection for lupus is one of its most essential treatments. It is so important I include sunscreen on my patients’ medication lists. It is specifically ultraviolet (UV) light that contacts the skin and increases lupus disease activity. UV light …